Today, I was stunned to see a press release for a new breastfeeding measurement tool, the MilkSense. From a research standpoint, I will admit that any handheld device that allows me to accurately measure milk transfer and is small enough to fit in my backpack makes me excited. Those highly accurate baby scales are heavy when they have to be moved by hand at altitudes greater than >10,000 feet. But, when I see devices like this, I, the researcher, want to be the product’s intended audience. Sadly, I, and other researchers, am never the target audience. It is always mothers. And that is a huge problem. Why? Because what devices like the MilkSense and the recently discontinued Milk Screen test strips actually serve to do is not to increase maternal confidence in the capacity to produce milk, but to call into question the ability of breastfeeding to meet an infant’s needs. Human milk and human babies evolved together, and hands
Anthrolactology Podcast
From all of us to all of you who read & follow us, Happy Holidays!! Also….we have some fun news!
The BeAT goes on: human milk maintains brown and beige adipose tissue in infants
Compared to most other, non-aquatic animals, we give birth to infants with relatively amounts of body fat. This has been hypothesized to explain why our infants can sustain a weight loss of 8-10% after birth while receiving immune factor rich colostrum. Infant body fat frequently increases across the first few months of life, and it is generally thought that this is in anticipation of nutritional stresses that may be associated with weaning and independent motor development (crawling, walking). However, baby fat is not all the same – babies actually have multiple different types of fat (also called adipose tissue). When it comes to BAT, BeAT, and babies, we actually know very little about the production and maintenance of BAT and BeAT (this is actually true for all ages). What can explain the differences seen in rates of BAT and BeAT decline in different infants based on the handful of studies? The answer may be BREAST MILK.
read more The BeAT goes on: human milk maintains brown and beige adipose tissue in infants
Nothing beats MOM: changing donor milk microbiota using an infant’s mother’s milk
In the neonatal intensive care unit, human milk is preferred food for preterm and very preterm infants. For very premature infants (less than 30 weeks), it is well established that human milk reduces the risk of necrotizing enterocolitis (NEC), a bacterial infection of the intestines with devasting consequences, and is associated with improved growth, cognitive development, and survival compared to infants receiving formula. There’s just one problem: donor milk, used when an premature infant’s mother’s own milk (MOM) is not available, generally consists of pooled and pasteurized milk from several donors. Donor milk – the second best food for premature infants after milk from the infant’s own mother – is suddenly missing one OR MORE of the factors in human milk that is thought to protect against NEC and other gastrointestinal infections. But, what would happen if you incubated donor milk with unpasteurized milk, from the infant’s own mother?
read more Nothing beats MOM: changing donor milk microbiota using an infant’s mother’s milk
Who manages the mammaries: physiology edition
and so I bring you “who manages the mammaries: physiology edition”, specially looking at how milk synthesis starts and milk supply is maintained. I think this will be useful for the overall trajectory of the multipart series emerging here. The onset of milk production occurs with lactogenesis. In humans, this is split into two general stages, the first occurring during the transition from pregnancy to lactation and the second characterized by secretory activation of the mammary gland. More than simply the onset of milk production, each discrete physiological phase hallmarks a number of important cellular changes within the mammary epithelium and the mammary ducts. The first phase, secretory differentiation, previously called lactogenesis I is followed by secretory activation, formerly known as lactogenesis 2, is characterized by a shift to full milk production and further cellular level changes (Neville et al., 2012). Secretory activation is usually complete within 72 hours following birth, however there is an increased incidence in delayed activation
Milk remembers: Immune factors in milk “remember” childhood environments – repost from Biomarkers & Milk
It is well established that with very few exceptions, human milk is the preferred first food for infants. While the benefits of breastfeeding/receiving human milk are considerable and influence the development of multiple systems in the infant, perhaps the best known benefits of human milk are its immunoprotective properties. Worldwide, breastfeeding is associated with reduced risk of infectious diseases in infants, and these protections persist even in highly hygienic conditions such as the United States (Bartick & Reinhold 2010). Many immune factors are found in human milk, including immune cells, cytokines that regulate immune responses, and secretory Immunoglobulin-A (sIgA), perhaps the most common immunoprotein in human milk. It is well established that there is considerable variation in the immune factors in milk between individual mothers and between populations. It is also known that many of the immune factors in milk are highly responsive, changing in response to active infection of either the mother or infant (blog post on this topic
Swirled or shaken? Does shaking actually damage milk – the scientific evidence (Repost from 2014)
Perhaps one of the most widespread pieces of advice women expressing milk will hear is about the best way to
Breastfeeding is the cornerstone of public health: a view from the milk
Breastfeeding belongs in our modern understanding of what public health is.
read more Breastfeeding is the cornerstone of public health: a view from the milk
Bringing Breastfeeding from the Past into the Present – by guest blogger Dr. Charlotte King
This month, Anthrolactology welcomes Dr. Charlotte King. Dr. King is a Postdoctoral Research Fellow at the University of Otago, New
New Year, New Book!
Our new book is here! Breastfeeding: New Anthropological Approaches is an edited volume featuring contributions by anthropologists working across the sub-fields. This book seeks to produce transformative knowledge and novel conversations about human lactation, breastfeeding, and human milk.
Repost: Pumping experiences survey, pt1
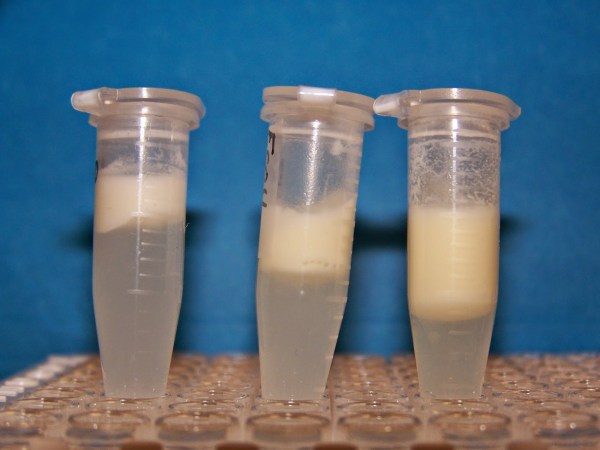
Pumping experiences survey – Post 1 of the Series First off, a giant THANK YOU to all the mothers who participated in the online survey. Your assistance was amazing! We started the pumping experiences survey to see how mothers would respond to differences in pump output, based on their normal pumping experiences. We had predicted that mothers who had dramatic changes in output in the experiment – either randomized to much more or much less than they typically produced – would have strong reactions to the images and the responses would tell us a lot about how women perceive their milk supply. The survey randomly assigned each mother to one of three images showing expressed breast milk– one photo showed 1 ounce of pumped milk, the second photo showed 6 ounces of milk, and the final photo showed 12+ ounces of milk. The volumes were classified as “low”, “intermediate”, and “high” volume. The photos created an experimental condition where
Announcing . . . Team Anthrolactology
We’re happy to announce that Anthrolactology is coming back to your regularly scheduled blogging. But, it is going to be EVEN BETTER!!
Support Safe Infant Feeding in Emergencies
In celebration of World Breastfeeding Week!! — Learn more at www.safelyfed.org
#WBW2016 #IYCFE #SafelyFed #helpmomsbreastfeed
#Breastfeeding saves lives.
In emergencies, the most important action a mother can take to protect her baby is to breastfeed. When breastfeeding is not possible, infants and young children need skilled infant feeding support.
Donations of money are essential to ensuring that NGOs can provide exactly the kind of breastfeeding support or supplies, foods, and resources needed to safely feed infants.
Donations of formula often go unused, are wasted, or are distributed improperly, which can have grave consequences for infants’ survival in emergencies.
Learn more about how to support infant and young child feeding for refugee and migrant families. Visit us on Facebook at https://www.facebook.com/safelyfed/ (Infant Feeding Support for Refugee Children).
Give today to a vetted organization that provides care for infant and young child feeding in emergencies in alignment with the World Health Organization standards. These include:
UNICEF http://www.unicef.org
Save the Children http://www.savethechildren.org
Nurture Project International http://nurtureprojectinternational.org
La Leche League Greece & Great Britain https://www.laleche.org.uk/donate
International Medical Corps https://internationalmedicalcorps.org/new/home
International Orthodox Christian Charities http://www.iocc.org
Emergency Nutrition Network http://www.ennonline.net
Children in Crisis
A video from the Infant Feeding Support for Refugee Children group.
#SafelyFed Refugee children in #Idomeni are in crisis. Learn how you can give donations of money to ensure that all infants – breastfed and non-breastfed – receive skilled support for safe nutrition in emergencies.
Infants and young children under 2 are especially vulnerable to illness, malnutrition, and death during humanitarian crises. According to the World Health Organization (WHO), in emergency situations artificial feeding increases the risk of death by diarrhoeal by 1300% as compared to breastfed infants. A baby may die within days of the onset of diarrhoeal disease. The younger the baby, the greater the risks of artificial feeding.
In this emergency, the transit context introduces serious challenges to safer formula feeding. Mass donations of powder formula, bottles, and teats increases the risks of infant death by diarrhea and malnutrition. This is because where refugee families are throughout Greece, they do not have access to the potable water, sanitation, or the supplies needed to properly prepare formula or scrub and sterilize bottles and teats.
UNICEF, WHO, WFP, International Medical Corps, and Save the Children have called for breastfeeding support and outline conditions for use of breast milk substitutes: http://www.unicef.org/media/media_57962.html
When artificial feeding is required, ready-to-feed (UHT) formula is recommended for infants less than 6 months. Non-breastfed infants more than 6 months and toddlers may have UHT milk or yogurt, along with healthy, age-appropriate complementary foods. Cup feeding is more hygienic than bottle feeding.
Breastfed infants should be exclusively breastfed for 6 months, and then breastfeeding should continue for as long as possible, up to two years and beyond. After 6 months breastfed infants may receive healthy, age-appropriate complementary foods. Relactation is possible for mothers who have stopped breastfeeding and wish to begin again. Cross-nursing (“wet nursing”) is recommended before offering breastmilk substitutes in emergencies. Formula should be used a last resort when all other options have been ruled out.
GIVE MONEY, NOT FORMULA OR BOTTLES to organizations providing infant and young child feeding aid. Donations of money allow them to purchase exactly the supplies needed, when needed, to deliver infant feeding support that does not put infants at further risk.
Learn about the IFE Core Group recommendations for supporting families with infants and young children in transit.
These recommendations have been translated into easy-to-use documents for aid workers and families: http://safelyfed.org/resources/
It Could Be Any One of Us
Re-blogging this post on the importance of infant feeding support in emergencies , by Brooke Bauer of Nurture Project International.